
Advancing Behavioral Health Services
For all patient-related inquiries regarding Marian's Outpatient Psychiatric Unit, please contact (805) 614-5620.
The Outpatient Psychiatric Unit is an integral part of the behavioral health service continuum, whose mission is to heal, comfort, and promote mental and emotional health for our patients. The purpose of this eight-bed unit is to provide our patients with urgent psychiatric evaluation and treatment in a therapeutic environment conducive to wellness and recovery. This unit serves to avoid the more confined structure of a standard emergency department and to offer an open design that allows patients to move about freely, helping reduce stress.
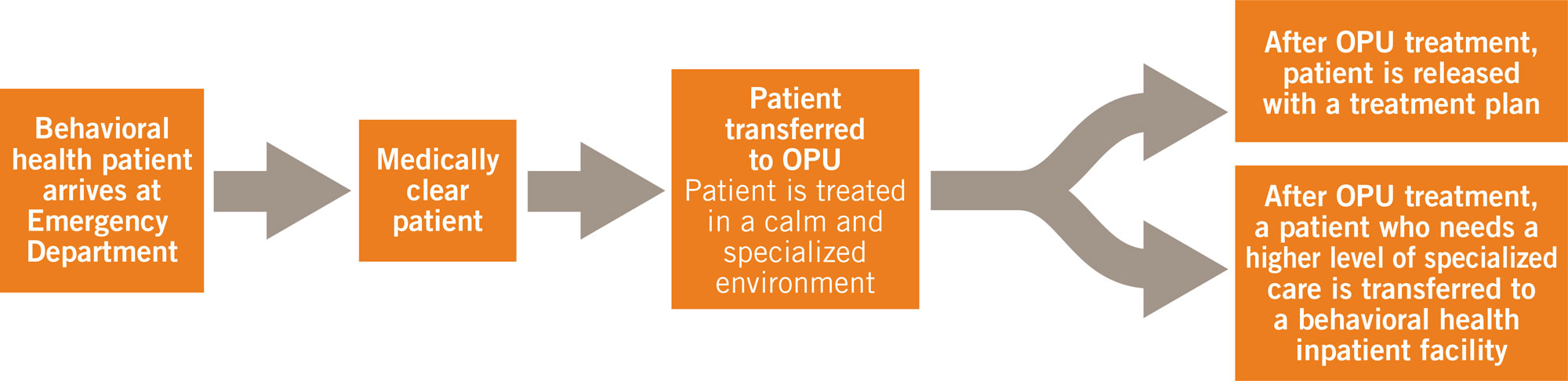
More than 61,200 patients are seen annually (or 170 patients every day) at Marian’s Emergency Services Department (ED). Improvements in facilities will shorten ED wait times for behavioral health patients by facilitating a smooth, safe, and speedy transition from the ED to the OPU.
The establishment of the OPU has provided access to all members of the community, assisting families that lack the resources to address a mental health need. In an area that has one in five households living below the poverty line and nearly 40% of the patient population comprised of migrant farm workers, traveling out of the area for care is straining. With the OPU, Marian has been able to decrease the need for inpatient transfers outside of Northern Santa Barbara County, treating patients in a familiar area they call home.
Additionally, the OPU allows behavioral health experts to work promptly with those in need, rather than having patients spend extended periods in Marian’s Emergency Department, waiting to be transferred to a behavioral health inpatient bed out of the area.
Click the button above to complete your one-time or recurring donation - you will be prompted to enter your payment information on the following screen. If you are making a recurring donation, kindly note: I authorize the Marian Regional Medical Center Foundation to use my credit card for future payments. I understand I may cancel this authorization at any time.